J Biomed 2018; 3:26-31. doi:10.7150/jbm.23594 This volume Cite
Research Paper
Outcomes of Epidural Neuroplasty Utilizing Adhesiolysis by Means of Hydraulic and Mechanical force
1. Department of Neurosurgery, Wan Fang Hospital, Taipei Medical University, No. 111, Section 3, Xinglong Road, Wenshan District, Taipei City 116, Taiwan
2. Graduate Institute of Injury Prevention and Control, Taipei Medical University, No.250, Wuxing Street, Xinyi District, Taipei City 110, Taiwan
3. Graduate Institute of Sports Science, College of Exercise and Health Sciences, National Taiwan Sport University, Taoyuan City, Taiwan
*Isao Aoi and Huan-Chieh Chen made equal contribution to this article
Abstract
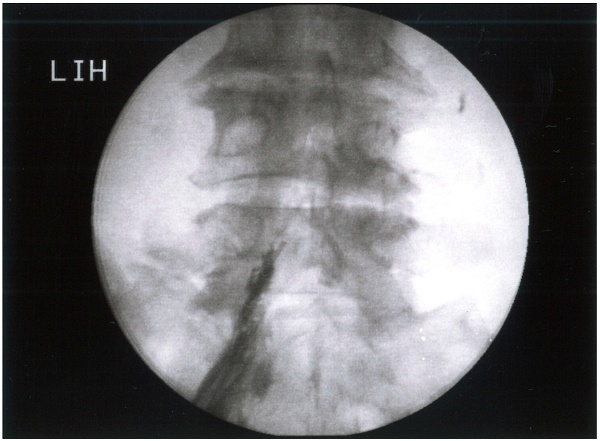
Background: Sciatica due to contained herniated discs can be managed with epidural neuroplasty which has emerged as a minimally invasive technique for the treatment of low back pain. Epiduroscopy also provides an alternative minimally invasive technique that offers diagnostic and therapeutic advantages. However, both procedures are not free of complications. The most commonly seen complications are related to the drugs and hypertonic fluid administered. The aim of this retrospective study is to evaluate the efficacy of epidural neuroplasty in the treatment of degenerative chronic low back pain and radiculopathy, and the prevention of complications by means of hydraulic and mechanical adhesiolysis with Cordis® catheter.
Methods: 112 patients treated by epidural neuroplasty were included in our retrospective, non-randomized case series. The outcomes and complications of epidural neuroplasty by hydraulic and mechanical adhesiolysis in patients with chronic low back pain or nerve irritation due to nerve root compression by a single-level, contained herniated disc were assessed. A blinded investigator assessed the patients before and at 3, 6, and 12 months after treatment. Patients were asked to quantify their pain using the visual analog scale (VAS) and were also surveyed in regards to their pain medication usage. The Oswestry Disability Index (ODI) was quantified by third-party observers. Observed data at 3, 6, and 12 months after management were matched to baseline.
Results: The level of pain intensity and medication usage lessened considerably in the first three months after the management. An improvement in functional status was also observed in the first 3 months. Pain scores and medication use continued to increase and functional status continued to decline in our patients over the 12-month follow-up period. There were no procedure-related complications observed.
Conclusion: This retrospective study of mechanical adhesiolysis with Cordis® catheter demonstrated a statistically significant improvement in VAS pain scores, functional status and a reduction in medication intake. These findings suggest that epidural neuroplasty can be a safe and effective procedure for selected patients. To evaluate the long-term efficacy of this minimally invasive technique, further randomized, controlled studies are required.
Keywords: Mechanical adhesiolysis, discectomy, disc herniation, low back pain, minimally invasive, caudal neuroplasty, epidurolysis